Home
A comprehensive resource for safe and responsible laser use
China: Laser pointers "regularly" harm children's eyes
It notes that an 8-year-old boy playing with a laser pointer suffered irreversible retinal damage to his left eye.
The story says "such cases are not rare" at the Shanghai Xinshijie Eye Hospital.
It also says that a "study conducted by the national quality authority found 29.8 percent of children have had access to laser products, laser pointers being the most common." It is not known what other, non-pointer, laser products were included in the study.
According to the story, the "government has issued a warning to alert parents not to buy laser pointers as toys for their children, but they are still widely available in local stationery stores. Most laser pointers don’t come with safety alerts to warn of the dangers present." The story did not say whether this was a national, provincial or local government warning.
From Shine News (Shanghai Daily)
Japan: Boy who routinely stared into a laser pointer develops lesion in one eye
At the age of 11, he had normal 20/20 (1.0) vision in the left eye, but 20/100 vision (0.20) in the right. Examination of the right eye showed a yellow lesion or fibrous tissue surrounded by a subretinal hemorrhage in the right macula. At age 13, examination showed the lesion was leaking on fluorescein angiography. At age 14, there was no change.
The doctors elected not to perform any treatment due to the patient’s age and mental condition.
From “Choroidal Neovascularization in a Child Following Laser Pointer-Induced Macular Injury”, Fujinami, K., Yokoi, T., Hiraoka, M. et al. Japanese Journal of Ophthalmology November 2010, Vol. 54, Issue 6, pp 631-633 (2010) 54: 631. https://doi.org/10.1007/s10384-010-0876-z First online January 21 2011.
Greece: 9-year-old "repeatedly gazing" into laser causes hole in his eye
The most serious injury that the boy caused was a large hole in his macula, shown with the yellow arrows.
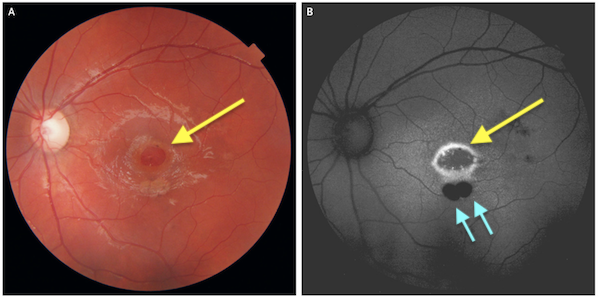
Two other areas of injury were not immediately visible in a funduscopic exam of the retina (photo A, using ordinary white light) but were clearly visible using fundus autofluorescence imaging (blue arrows in photo B, using a narrow wavelength of light). The round area to the left in both photos is the optic disc, a natural feature where the optic nerve begins — it is not laser damage.
The macula is where central vision occurs. The fact that the injury occurred in the macula indicates that the boy looked directly into the laser light with his left eye. Damage to the macula is serious as this area provides high resolution, color vision in the center of the visual field.
The injury reduced the boy’s vision to 20/100 in the injured left eye; his right eye remained at 20/20. The boy’s ophthalmologists felt the hole was too large and too much time had passed since the injury for surgery. (The doctors suspected that the boy had injured his eye at least a year earlier.) Because surgery might make things worse, causing a cataract without improving the macula, they “favored conservative management.”
There was no improvement in vision even 1 1/2 years after the injury was first presented to the ophthalmologists.
The power of the laser pointer, and other details of the incident, were not described in the one-paragraph report published June 21 2018. One of the authors told CNN the boy’s father “had bought the laser as a toy from a street merchant.”
From the New England Journal of Medicine (N Engl J Med 2018; 378:2420, DOI: 10.1056/NEJMicm1714488) Authors: Sofia Androudi, M.D., Ph.D., and Eleni Papageorgiou, M.D., Ph.D. Additional reporting by CNN. This story was picked up by many other news sites around the world.
US: Study examines four laser-caused eye injuries in children, at one medical practice
In a separate interview, one of the authors, ophthalmologist Dr. David Almeida, said these cases are “happening more frequently…. It was previously thought this was a one-in-a-million event. It's still probably a rare-to-uncommon reaction, but it's not a never reaction.”
All four children had foveal laser burns. Three of the children had potentially permanent vision loss. These are the cases:
- A 12-year-old boy looked into a green laser pointer for about a minute. He had decreased central vision in both eyes, with 20/20 vision in one eye and 20/30 in another. His vision and macular condition was found to be unchanged after 7 months.
- A 16-year-old teenager similarly had central vision loss in both eyes, after playing with a green laser pointer for about 30 seconds. He was first examined three days after the exposure, scars and atrophy were found on the retina. Two weeks later his vision has worsened. Visual acuity was 20/40 in both eyes with no improvement.
- A 9-year-old boy looked at the reflection of a green laser pointer in a mirror (essentially the same as a direct beam) for an unknown length of time. His vision was 20/50. He was treated with 1% prednisolone three times a day for two weeks. His vision improved to 20/30, but he still had “persistent abnormalities of the photoreceptors.”
- A 12-year-old boy looked into a red laser pointer for about 15 seconds. He had central vision loss, and 20/70 vision. He was given an injection of bevacizumab, which gradually improved his vision and symptoms. After 1 year, he had 20/20 vision.
The authors noted that laser pointers are more available, that users may not be aware of the dangers, and that some users may use pointers improperly.
Visible lasers less than 5 milliwatts (the U.S. legal standard for a laser to be marketed as a “pointer”) are considered to be generally safe due to the bright light reflex, which causes a person to blink and turn away from a bright light. So one question is why these children were injured by laser pointers.
One reason, according to the authors, is that “children increase their chance to retinal injury by staring at the laser beam without blinking or averting the eye for a prolonged duration.”
Another possible cause is that “the labeling of the power output of a laser point may be different from the device’s actual specifications.” They referred to a study of 122 laser pointers, where 90% of green pointers and 44% of red pointers were above the 5 milliwatt U.S. legal limit.
The study said that treatment options were “limited and also controversial.” Use of corticosteroids has shown “mixed results.” It may be enough to observe a patient over time, since many injuries will stabilize.
The authors recommended that laser pointer hazards “should be communicated to health professionals, school teachers, and guardians in an attempt to raise the public awareness of this emerging public health issue. Unsupervised use of these laser pointer devices among children should be discouraged, and there is a need for legislation to limit these devices in the pediatric population.”
From Retinal Injury Secondary to Laser Pointers in Pediatric Patients, Kunyong Xu, Eric K. Chin, Polly A. Quiram, John B. Davies, D. Wilkin Parke III and David R.P. Almeida, in Pediatrics; originally published online September 1, 2016; DOI: 10.1542/peds.2016-1188. A general interest article summarizing the study, with additional comments from Almeida and another ophthalmologist, is at HealthDay.com. The abstract of the Pediatrics article is below; click the “Read More…” link.
Click to read more...
UK: Journal report of five children injured by laser pens
According to the abstract, “Clinically, three children had an acute vitelliform-like maculopathy which resolved to leave sub-foveal retinal pigment epithelium changes with reduced vision. One case was complicated by a choroidal neovascular membrane.”
- Case 1 was of a nine-year-old boy who on December 22 2013 was tested with normal vision of 6/5 (U.S. 20/17 -- better than 20/20) but on December 26 complained of vision loss and was found to have 6/12 (20/40) in the left eye and 6/15 (20/50) in the right eye. The family said he was given a laser pointer as a “toy” and had been playing with it on Christmas Day. The child denied looking directly into the laser beam. The family had three laser pens: a 57 mW blue 405nm, a 42 mW green 532 nm, and a 72 mW red 650nm. All exceeded the British Standard of 5 mW for a Class 3R laser. The boy was prescribed steroids. Nine months after the initial complaint, the best corrected vision was 6/9.5 (20/32), and optical coherence tomography showed persistent outer retinal layer disruption at the fovea. [The boy was later identified in press coverage as William Jackson, from Wadsley. Details are at The Star.]
- Case 2 was of an 11-year-old boy. He had decreased vision in both eyes of 6/7.5 (20/25). Eight weeks later he had sub-foveal retinal pigment epithelium changes. His vision was 6/12 (20/40) in the right eye and 6/15 (20/50) in the left eye. He said that a friend had aimed a laser into both of his eyes before the decreased vision occurred. The doctors were not able to examine what they characterized as the laser “toy”.
- Case 3 was of a 15-year-old girl. She aimed a laser pen into both eyes for 30 seconds. The next day she had scotomas (vision loss or spots) in both eyes. Her right eye was 6/7.5 (20/25) and her left eye was 6/6 (20/20). Upon examination, a vitelliform-like maculopathy (abnormality in the macula or central vision area) was seen. She did not return for follow-up visits.
- Case 4 was of an 8-year-old boy who had reduced vision of 6/12 (20/40) in his right eye, and normal vision of 6/6 (20/20) in his left eye. The right fovea was seen to have retinal pigment epithelial changes “consistent with laser burns.” The boy admitted he had played with a laser pointer a few months before, but said he did not point it directly at his eye.
- Case 5 was of a 13-year-old boy who had noticed declining vision in his right eye. It was found to be 6/36 (20/120); his left eye was 6/6 (20/20). He admitted aiming a laser pointer into his right eye. A fibrosed choroidal neovascular membrane was found at the right fovea.
The authors noted that “The retinal damage reported following such injuries is variable. This is due to variety of laser powers and wavelengths as well as ocular factors such as fundal pigmentation, blink responses, pupil size, and proximity of the laser burn to the fovea. Assessment of alleged laser eye injury requires accurate history and examination. Treatment for such laser retinal injuries is uncertain. Oral corticosteroids are sometimes administered.”
The authors stated that some laser devices are marketed as “toys”. They said they are aware of other children in the U.K. with retinal injuries from imported laser pointers. They conclude: “We suggest that children should not be given laser pointers as toys.”
From “‘Toy’ laser macular burns in children”, in Eye (2014) 1-4, by N. Raoof, TKJ Chan, NK Rogers, W Abdullah, I Haq, SP Kelly and FM Quhill. A downloadable PDF version is here. A story from the Bolton News gives some additional comments from author SP Kelly.
US: Child suffers eye injuries from adult misusing high-powered blue laser
The case was reported in JAMA Ophthalmalogy under the title “Ocular Safety of Recreational Lasers.” Authors Glenn Yiu, Sujit Itty and Cynthia Toth are with the Department of Ophthalmology at Duke University Medical Center in Durham, North Carolina.
They described the boy’s injuries as being caused by a Spyder III Pro Arctic “a class 4, high-powered 1250 mW laser that is manufactured from the 445 nm blue diode of a dismantled home theater projector and that is commercially available for online purchase from overseas.” This brand of laser is manufactured by the company Wicked Lasers; an 800 mW version was reviewed here.
In the case they described, “the adult directed the laser at the child’s eyes in jest, unaware of the harmful consequences.”

A copy of the safety label that appears on a Wicked Laser Spyder III Pro Arctic, containing the IEC and U.S. FDA-mandated wording for a Class 4 laser: “Avoid eye or skin exposure to direct or scattered radiation”
According to the authors, “imaging studies suggest that the laser damage was limited to superficial retinal vessels with no involvement of the underlying retinal pigment epithelium or choroid. To our knowledge, this is the first report of a continuous wave laser in the visible spectrum–damaging retinal vessels without affecting the retinal pigment epithelium, the site where damage from visible lasers typically occurs.”
They speculate that this may be caused by greater absorption of shorter wavelength lasers by hemoglobin, or a defocusing of the laser due to chromatic aberration and myopia in a child.
The authors conclude that “with the expanding use of lasers in nonoccupational or recreational settings, escalation of laser safety awareness and consumer laser regulations is paramount to prevent future ocular laser injuries.”
From JAMA Ophthalmology, published online January 09, 2014. doi:10.1001/jamaophthalmol.2013.5647. Thanks to Dr. David Hunter for bringing this to our attention.