Home
A comprehensive resource for safe and responsible laser use
If you are hit by a laser beam
Laser injury expert Bruce Stuck, director of the U.S. Army Medical Research Detachment of the Walter Reed Army Institute of Research at Brooks Air Force Base.
Note that before going to a doctor, you may want to call police or relevant authorities if the incident was serious or poses a threat to others. For more information, see the “To report an incident” page.
Topics
-
How much laser light can cause an injury?
- Whether laser exposure to your eye will result in an injury depends on a number of factors. These include:
- the power of the beam
- the divergence (beam spread)
- distance from the beam (how much the beam was able to spread before going into your eye)
- wavelength of the laser (different colors and wavelengths affect different parts of the eye)
- time of exposure (how long it was in the eye)
- movement of the laser light across the eye (did it stay on one spot, or did it quickly scan over the eye)
- which eye structure(s) absorbed the laser light (retina for visible light, cornea or lens for infrared or ultraviolet)
- location of the laser light on the eye (e.g., central vision vs. peripheral vision)
- whether the laser light was created continuously (CW) or was pulsed
In many cases, you may not have access to the laser which caused an exposure — so you would not know the power of the laser. Even if there is a label on the laser, stating either the maximum power or the laser’s Class, the label may be incorrect. If at all possible, retain the laser so its output power and characteristics can be tested.
More information is in the FAQ answer to the question, “When does a laser pointer get powerful enough to be dangerous?” -
What is an eye injury?
- For visible light exposures such as from laser pointers or shows, the only part of the eye that can be damaged is the retina. A lesion or scotoma on the retina is rightfully termed a “laser eye injury” or “laser eye damage”.
In contrast, if a person has afterimages, or a physical reaction, or rubs their eyes, these are NOT injuries. They are “laser exposure effects” or “post-exposure effects”.
It would be inaccurate for a newspaper to report that a pilot was “injured” by a laser if they did not have the spots or retinal lesions which indicate true injuries. An accurate description would be that the pilot was “affected” by the laser light, and then list the particular effects reported (afterimages, headache, photophobia, dry eye, watering eye, corneal abrasion, etc.). -
Is flashblindness an eye injury?
- The short answer is no, flashblindness is not an injury. It goes away with no permanent effects.
If you were exposed in the eye to a strong direct laser beam, you may have temporary flashblindness with an afterimage spot. (These are two sides of the same coin. Flashblindness causes temporary afterimages, and having an afterimage that eventually fades means you were flashblinded.)
Some news reports and government officials have claimed that persons were "injured" by being temporarily flashblinded. But assuming the persons have no permanent change to their vision, then by definition they were not injured. (And it is not possible to be permanently flashblinded. A permanent injury is just that, an "injury", not "flashblindness.")
An afterimage is the eye’s normal response to overly bright light. It is similar to what happens after looking directly into a camera flash. If flashblindness WAS an injury, that would mean than any photographer using a strong camera flash to illuminate a person would be "injuring" them — clearly not true.
The afterimage area looks like a blob if you looked directly at the light, or can look like separate spots or a line if the eye was moving during the exposure.
Afterimages take about 5 or 10 minutes to fade. If after this time the spots are still visible, you may have retinal damage. Fortunately, this often heals within a few days or weeks. This is similar to how your skin heals after getting a small cut or a bruise. Vision may return completely to normal, or you may have faint spots noticeable only under special conditions such as looking at a uniform white wall or blue sky. An Amsler Grid test can help in finding small lesions within 8-10 degrees of the fovea.Technical definition of afterimages vs. laser eye injuries
Technically, afterimages are not injuries. They are caused by saturation of rhodopsin or "bleaching" in the outer segments of photoreceptors that results in a localized reduced sensitivity.
In contrast, an injury results in a minimally visible lesion which histologically involves the retinal pigmented epithelium and the photoreceptors. -
Other post-exposure effects, and self-caused injuries
- Sometimes, persons surprised by bright lasers report a physical reaction such as feeling “hit” or stunned. They may have a headache afterwards. They may report extra-sensitivity to light. They may also have watery eyes, or report having dry eyes.
Post-exposure examinations sometimes find “corneal abrasions”. Since visible laser light passes through the cornea and is not absorbed, the abrasions had to come from rubbing their eyes after the incident.
Therefore, after exposure to a bright visible laser, avoid rubbing your eye. If it is watering, you can dab it with a tissue. -
If you have been lased: Guidance from the U.S. Air Force
- The following statement is from the U.S. Air Force Laser Injury Guidebook. It is a guide that can be read to a pilot, or any person who has been exposed to laser light. We have changed one word which was ambiguous (from “injuries” to “exposures” in sentence 4).
If you have been involved in a laser incident, then naturally you are concerned about what effect the laser might have had on your eyes and vision. If you can read 20/20 and there is no distortion on the Amsler grid test, then it is unlikely that the laser did any significant damage. In fact, it may have done none at all.
Laser exposures can have a wide range of effects including flash blindness, dazzle, dark spots, hazy vision, floaters, burns, retinal bleeding, etc. Of special interest are the hazards posed by visible lasers from glare and flash blindness, and from very high energy lasers that could cause serious thermal injuries. Luckily, the part of the eye responsible for most of our central vision is about the size of a pinhead. It is possible, that this area could be damaged by a laser, but only if a person happened to be looking directly at the light. A laser injury even a few millimeters away from this area, will probably not significantly affect the central vision. The central vision is what you use to read, watch TV, and drive.
Most people after encountering a laser incident quite naturally start to become overly conscious about how their eyes feel and sometimes begin to rub their eyes. This has caused some people to erroneously conclude that their eye was injured. Furthermore, rubbing of the eyes can produce small scratches on the cornea resulting in painful irritated eyes. The important point is that if your vision and eyes seem normal after direct laser beam exposure, then there is probably no significant damage to your eyes due to the laser beam. -
Self-test from the U.K. Civil Aviation Authority
- The U.K. Civil Aviation Authority have produced an “Aviation Laser Exposure Self-Assessment”, to be used by persons exposed to laser light. The ALESA card is available in hard copy, and can also be downloaded from CAA’s website. If downloaded, the Amsler Grid on the first page should be printed so it is 10 x 10 cm, or 4 x 4 in.

Click either image for the PDF version stored locally at LaserPointerSafety.com. This may be different from the version currently at CAA’s website.When staring at the dot in the center of the grid, if the lines appear distorted or there are blank or faded areas, there may be a problem. The person is encouraged to remove themselves from aviation-related duties such as flying or air traffic control, and to see an eye specialist.
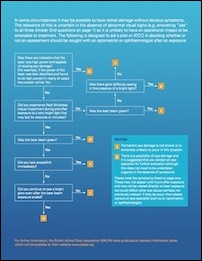
The second page has a flowchart of exposure conditions leading either to a “1” meaning unlikely eye damage or a “2” meaning eye damage possibility. If the person scores a “2”, the flowchart suggests they see an eye specialist.
Commentary from LaserPointerSafety.com: In our opinion, the flowchart could lead to many unneeded worries. For example, there is a question about whether “you continue to see a bright glow even after the laser beam exposure ended.” If Yes, it is suggested to have an eye exam. But by this standard, anyone having a bright spot after being photographed using a camera flash should have an eye exam. In our view, if you get a “2” on the flowchart, do not worry unless you also have any new symptoms or indications of a change in your vision. If you pass the Amsler Grid and otherwise have no visual changes or problems, the laser exposure has not changed your vision. This is echoed by the U.S. Air Force guidance in the previous section. -
See a specialist
- If you have spots that have not faded, or if you have any concern at all about effects or injuries from a laser incident, you should consult with a vision specialist. For inspection of the eye and retina (looking for damage), either of these two types of specialists would be fine:
- Ophthalmologist: This is a medical doctor specializing in the eye.
- Optometrist: This is an eye care specialist usually focused on glasses, contacts and routine eye care screening (glaucoma, cataracts).
If your situation requires more specialized care, you may be referred to a retina specialist:- Retina specialist: This is an ophthalmologist (medical doctor) who specializes in diseases and disorders of the retina. If you live in an area with a number of specialists, try to find one with experience with laser/retina interactions.
-
Diagnosis
- The following is from the journal article “Assessment of Alleged Retinal Laser Injuries”:
Six Questions That Facilitate the Diagnosis of Alleged Retinal Laser Injuries- Are there ocular abnormalities that could have been caused by a known laser-tissue interaction at the time of the reported incident?
- If the answer to 1 is “yes,” have those abnormalities been documented by a reliable technique, such as fundus photography, fluorescein angiography, or optical coherence tomography?
- If the answers to 1 and 2 are “yes,” do findings from ophthalmoscopy and retinal imaging evolve after the incident in a manner consistent with a laser injury?
- If the answer to 1 is “yes” and substantial visual or somatic complaints are present, is there any scientific evidence that the objective ocular findings could cause the reported subjective complaints?
- If the answer to 1 is “yes” and substantial visual complaints are present, is the location of Amsler grid or visual field defects stable and consistent with the location of the retinal abnormalities supposedly responsible for causing them?
- If the laser source involved in the alleged injury is available or known, is it capable of producing the observed clinical findings under the reported exposure conditions?
If the answers to all six questions are “yes,” then a laser injury has almost certainly occurred. The authors state that “perceived ocular injuries with no demonstrable tissue damage are not real laser injuries.” In their concluding “Comment” section, the authors state that injuries that cause serious visual problems are readily apparent from tests, while injuries that are subtle or ambiguous “should have excellent visual prognoses and clinical outcomes.” -
Injury descriptions
- The information below, about four general types of incidents and injuries, comes from a 1990 pamphlet, U.S. Army field manual “FM 8-50, Prevention and Medical Management of Laser Injuries”. Additional commentary is from LaserPointerSafety.com (LPS).
Bright light/glare
- Patient-reported symptoms: Temporary loss of vision. Bright light experience. No pain.
- Eye exam results: Normal eye
- Diagnosis/cause: Glare, dazzle or temporary flashblindness from visible laser. (Note: infrared and ultraviolet laser beams are not visible and thus by definition cannot cause glare, dazzle or flashblindness.)
- LPS Commentary: This is not cause for eye health concern. The only concern is if the bright light impairs a critical function, such as a pilot who is exposed to laser light on landing, or the driver of a motor vehicle.
Minor injury
- Patient-reported symptoms: No or slight visual impairment. Dark spot in field of vision.
- Eye exam results: Non-foveal retinal lesion(s). [This means there is a spot or spots visible on the retina. The spot(s) are not located in the small central (foveal) vision area, but are elsewhere in the visual field.]
- Diagnosis/cause: Small non-foveal retinal burn(s) with no or minimal hemorrhage [bleeding].
- LPS Commentary: For the Army, this is not serious. A soldier with these symptoms would be returned to duty without seeing a physician. It is likely that such an injury would heal with no noticeable effect on normal vision.
Serious injury
- Patient-reported symptoms: Vision impaired. Large dark spot at or near center of vision.
- Eye exam results: Foveal retinal lesion(s)
- Diagnosis/cause: Perifoveal retinal burn and/or hemorrhage [bleeding].
- LPS Commentary: This is more serious because the spot is at or close to the center of vision. The fovea is the central 2 percent of vision, about the width of a word or two read at arm’s length. When we look directly at something, we are using foveal vision. Loss in this area is thus more serious.
Severe injury
- Patient-reported symptoms: Severe visual impairment. Large dark spot at or near center of vision. Large floating objects in eye. May see blood [visual field is red].
- Eye exam results: Foveal retinal lesion(s) which may be obscured by vitreous hemorrhage.
- Diagnosis/cause: Foveal retinal burn, with vitreous or subretinal hemorrhage.
- LPS Commentary: Such severe symptoms are unlikely to be caused by accidental, brief exposure to lasers generally available to consumers and the general public. Such injuries could be caused by deliberate staring exposure self-inflicted by a child or a drunk person. There have been a very few severe injury incidents (three times in 30 years) at light shows when pulsed lasers were illegally and incorrectly used for audience scanning.
-
What vision loss can occur?
- Sometimes laser pointer injuries are incorrectly characterized as causing “blindness” when the person actually has some visual ability.
Below are recommended levels to use when discussing vision loss. These levels, and their effect on vision and functional ability, are described in detail in a 2002 report prepared for the International Council of Ophthalmology entitled “Visual Standards – Aspects and Ranges of Vision Loss.”
1. NORMAL VISION
2. LOW VISION (“Lesser degrees of vision loss, where individuals can be helped significantly by vision enhancement aids and devices.”)
2a: Minimal vision loss
2b: Mild vision loss
2c: Moderate vision loss
2d: Severe vision loss
3. BLINDNESS (“Total vision loss and conditions where individuals have to rely predominantly on vision substitution skills.”)
3a: Profound vision loss
3b: Near-total vision loss (near blindness)
3c: Total vision loss (total blindness) -
Treatment
- In 2014, LaserPointerSafety.com consulted two experts regarding potential treatments for a retinal burn (no hole, and no hemorrhage, just a white burn). They stated the following:
- Symptoms and vision will probably improve over time. The conservative approach would be to treat with oral NSAIDs (non-steroidal anti-inflammatory drugs) such as ibuprofen or indomethcin. More aggressive therapy has been used, and outcomes are often good, only a small reduction in vision and small scotoma, in individual accident cases. Steroids, oral and/or steroid injections in the eye have even used. Anti-VEGFs (ranibizumab, bevacizumab, pegaptanib, and aflibercept) injected in the eye have promise for some conditions that have similarities to laser eye damage. The outcomes of these laser injuries may have been similar without treatment. The side effects of more aggressive treatment should be considered.
- Treatment should begin after the injury, ideally within the first day or two. Fortunately, since lesions seem to remain active for days or even weeks after the exposure, even late treatment -- starting days or even weeks later -- would still be beneficial.
- Surgery should be reserved for more complicated cases. Stem cells are used and work for some corneal damage, but for the retina stem cells are for the future. Growing healthy retina to replace damaged retina is appealing and maybe someday that will be a standard treatment.
- One or more follow-up exams should be scheduled. These are important “for many different reasons.”
Other treatment information
U.S. Army field manual FM 8-50, written in 1990, says the following about retinal injuries:- “A patient diagnosed with a laser retinal injury is evacuated to a hospital where he can be examined by an ophthalmologist. Currently, there is no proven treatment of retinal laser lesions except for surgical intervention (vitrectomy) for severe vitreous hemorrhage [retinal bleeding -- the patient would notice red in the visual field].... NOTE: Retinal burns do not require eye patches. They only make the patient more disabled by taking away all of his vision; thus, further emphasizing his injury.”
Do not be upset by the reference to surgery. This would only be undertaken for massive injury which includes severe bleeding. The victim would see red in their visual field. Such a severe injury from laser pointers or audience exposure to light show lasers is extremely unlikely.
Army field manual FM 8-50 also says this about the stress that can come as a result of a retinal injury:- “Laser injuries may be especially stressful; vision is one of our primary means of relating to the world about us; and the fact or prospect of being deprived of vision will be a source of fear.... Medical management of stress reactions for patients suffering from real or imagined laser injuries is like stress management of other injuries. Repeat the reassurance that symptoms will improve with rest, nutrition, hygiene, and the expectancy of an early return to the soldier’s unit.”
The Rodney Hollifield source noted below (chapter 25) states that as of 2003, steroids have been considered for retinal treatment but are not proven to work:- “To date, there are no proven medical interventions for the treatment of laser injuries involving the retina. The use of intravenous steroids in the acute setting to limit subsequent epiretinal and subretinal fibrosis is controversial and unproven to date. Intravitreal injection of tissue thromboplastin activator (TPA) has been successful in removing subfoveal blood.”
See also this study, apparently from around September 2004, stating “Caution urged in steroid treatment for laser retinal injuries”, about research by Stephen T. Schuschereba.
However, a 2007 study, “New approaches to the diagnosis and management of laser eye injuries” did find benefits from steroids:- “The emergence of high resolution optical coherence tomography (OCT) along with evidence showing beneficial effects of anti-inflammatory drugs for retinal edema and neovascularization suggests a rational plan for the diagnosis and management of patients with acute laser eye injury.... The use of anti-inflammatory medication may enhance the initial recovery of vision and reduce the likelihood of longer term retinal complications from scarring and neovascularization.”
In addition, a 2004 study, “DARPA Soldier Self Care: Rapid Healing of Laser Eye Injuries with Light Emitting Diode Technology”, indicates that “photobiomodulation” treatment with LEDs may be beneficial. You may wish to share the study with your eye care professional. This is the concluding paragraph:- “The results of this study and others suggest that photobiomodulation with red to near infrared light augments recovery pathways promoting neuronal viability and restoring neuronal function following injury. Importantly, there was no evidence of damage to the normal retina following 670 nm LED treatment. Based on these findings, we suggest that photobiomodulation may represent an innovative and novel therapeutic approach for the treatment of retinal injury as well as the treatment of retinal diseases, including age-related macular degeneration, glaucoma, diabetic retinopathy, and Leber’s hereditary optic neuropathy.”
-
If you were at a laser light show
- Professional laser light shows are intended to safely scan into the audience. At audience scanning shows there will be occasional “hits” to the eye, but as long as there is no afterimage, the light level should be safe.
If you experience uncomfortable light levels or long-lasting afterimages, you should take simple actions to avoid the direct laser beams. Fortunately, even in such a case of brighter shows, injury reports from continuous-wave lasers are extremely rare.
Three shows over the past decades have stupidly and illegally scanned pulsed lasers into audiences. This caused approximately 50 total injuries in the three incidents. However, all responsible laserists know that they must never use pulsed-type lasers for audience scanning.
There also was a claim of audience injuries, initially attributed to a laser show, which turned out to be due to irresponsible laser pointer misuse by audience members attending the laser show.
If you want to report an unsafe laser light show, see this page.
Many more details about laser light show injuries (real and claimed) are available on the page Injury from a light show laser? This page also has a link to a 31-page paper about audience scanning.
For information about how outdoor laser shows operate to protect pilots’ vision, see the ILDA page. -
Baseline eye exam? (before working with lasers)
- For people who are hired to work with lasers, a baseline eye exam may be useful.
The ANSI Z136.1 "Safe Use of Lasers" standard does not make this mandatory ("shall") but does say that it "should" be required for laser personnel exposed to Class 3B and Class 4 lasers. Usually it is at the discretion of the company or institution whether to perform or require a baseline exam. Of course, anyone can make a personal appointment with an ophthalmologist to check the condition of their eyes and retina, and to have retinal photographs taken and retained.
According to a March 8 2019 Air Force press release, "the DOD 6.055.05-Occupational Medical Examinations and Surveillance Manual [states that] laser workers are considered to be at a high risk of accidental exposure due to their continuous involvement with a laser system. Workers are required to complete multiple visual tests before qualifications are given.
The press release quotes an Air Force optometry flight chief as saying “What we would like to see during the exam is someone who is seeing 20/20 far and near, their intraocular pressures are normal and they’re not having any color deficiencies in either eye. We also want to make sure that the retina is responding normally and that there are no missing pieces or vision distortion.”
The baseline exam serves two purposes:- It can be "used to determine whether or not an individual is capable of working in a laser environment or if it would endanger them of completely losing sight." Quoting the optometry flight chief, “Let’s say that the best they could see during the initial test was 20/100 and they could only see monocularly for example. If something happened to the one good eye that they had, that’s it.”
- If after working with the laser there is a laser exposure or the person develops vision problems, "[t]he previous documentation can help the clinic conclude what is wrong with the patient and can inform the doctor on what actions need to be taken to provide treatment."
-
Lasers causing heat on the skin
- Visible laser beams are concentrated light, so they also can cause heat and burns on skin. There are many factors that determine whether one can feel, or can be burned, by a visible-light laser.
- Power of the laser. The higher the power, the greater the potential for heating and burning.
- Concentration (irradiance) of the laser light. A focused beam will be felt sooner than if the same beam is spread out. The spreading can be done by a lens or simply by distance. The farther away a person is from the laser source, the more the beam spreads and (if handheld) the harder it is to keep the beam on a single spot.
- Wavelength (color) of the laser light. For visible wavelengths, violet is absorbed most strongly, red the least. There are mid-range peaks of absorption around 532 nm (green) an 585 nm (yellow).
- Laser power generation: pulsed vs. continuous wave. Almost all handheld lasers, including pointers, emit light continuously. Fortunately, these are less hazardous than lasers that emit the same amount of total power but which do it in very short pulses. For continuous wave lasers, the main damage mechanism is thermal — similar to a constant flame. For pulsed lasers, the concentration of power in the pulse can cause instant steam explosions in the retina or skin, which are more damaging and painful. This website is primarily about continuous wave lasers emitting visible light (not ultraviolet, not infrared).
- Skin sensitivity. Some locations such as the lips, tongue and palm have many more nerve endings and are thus more sensitive than other parts of the body.
- Skin color (melanin). Darker skin will absorb more light energy, just as a dark-painted car's surface will be warmer than a light-painted car's surface.
Because of these factors, it is difficult to say what power of laser, at what distance, can be felt or can cause skin injury.
In general, very low power lasers such as 1 to 5 milliwatts cannot be felt. Lasers above 50 mW can be felt if the beam is left on the skin for a short time and at a close distance. Lasers above 500 mW are considered skin hazards since at close ranges they can cause instant skin burns.
There are two other important factors to consider.- One is that a person can think they feel heat, even when the light level is too low to be detected — or even if there is no actual light. In experiments published in 2007, subjects had low-level laser light shined on a rubber hand that was positioned over their own hand. Sixty-six percent of subjects reported heat or tactile sensations from the laser light — even though 1) the light was on a rubber hand, not their own and 2) the laser power was low enough that it would not noticeably heat up even on a real hand.
- The other factor is that some persons feel heat sensations and may even have skin marks or burns, when there is no plausible laser or other energy source nearby. They may feel that others are aiming lasers or energy rays at them, to harass them. Their feelings and experiences are real. However, these perceptions may be due to physical problems with nerves, brain or body. More discussion of this is on the page If you are harassed by lasers.
-
Non-laser eye problems
- Of course, eye problems can occur from natural causes. In August 2017, a person wrote to LaserPointerSafety.com, concerned about vision changes a few months after looking at diffuse light from a laser pico projector.
He wrote “I began to notice something was going wrong with the vision in my right eye. Street lights and car headlights started to appear unusually blurred and bloomy at night, sharpness of objects at a distance in the daytime dropped noticeably from my normal prescription (which itself had barely changed at all over the last 20 years prior to this), and it began to feel like there was constantly a foreign object in that eye.”
We consulted experts. They agreed that the light level was not bright enough to have caused the problem. One of the experts wrote the following:
Other causes of these vision changes should be investigated. Medications and health should be considered. Blurry vision and bloody lights at night could be caused by lens or retina problems. The pain sounds more like a corneal problem, foreign body or recurrent corneal erosion or possibly anterior uveitis. I would like to know his visual acuity, Amsler grid results, OCT, and maybe fluorescein angiography. If he is relatively young to middle aged, central chorioretinopathy (CSC) should be considered. That is a disease in which a serous detachment of the neurosensory retina occurs over an area of leakage from the choriocapillaris through the retinal pigment epithelium (RPE). Other causes for RPE leaks, such as choroidal neovascularization, inflammation, or tumors, should be ruled out to make the diagnosis.
The causes of CSC are not fully understood. It is thought that any systemic exposure to a corticosteroid drug can bring about or worsen CSC. Corticosteroids are found in allergy nose sprays and anti-inflammatory skin creams available over the counter, and are often prescribed to treat a variety of medical conditions.
Age-related macular degeneration is more likely in older patients. While that develops slowly symptoms can occur with over a short time. If associated with fluid the prognosis is worse.
Chronic long term diffuse reflection at these wavelengths would not be expected to cause photochemical damage to the retina.
Sudden blurry vision can have many etiologies.
An extensive exam is certainly indicated. -
Resources
- An excellent overview of laser eye injuries, detection and treatment is the article “Managing Retinal Injuries from Lasers” from the American Academy of Opthalmology’s EyeNet magazine.
Another good overview is “Laser Bio-effects” from the U.S. Department of Energy Berkeley Lab. This webpage discusses both visible-beam lasers and non-visible (infrared, ultraviolet) lasers. Be sure that the material you are reading is valid for the type of laser (visible, IR, UV) with which you are concerned. [Thanks to Emilien for this link]
An August 2004 article describes “Assessment of Alleged Retinal Laser Injuries”. The article, from Archives of Ophthalmology, is primarily for the ophthalmic professional, though they also give some interesting case studies.The authors note that “Accidental, intentional or clinical retinal laser lesions do not cause chronic eye, face, or head pains. Diagnosis of a retinal laser injury should be evidence based, not a matter of conjecture or speculation.”
Especially for pilots and flight surgeons, the U.S. Air Force School of Aerospace Medicine in 2008 produced a Laser Injury Guidebook. Similar to the above, it gives instructions for detecting and assessing claimed laser eye injuries.
An online resource for those not familiar with detection of retinal laser injuries is chapter 25 of “Ophthalmic Care of the Combat Casualty” by Rodney Hollifield. See the section on Diagnostic Modalities, page 435.
There is some information on injuries and treatment in “Laser Pointer Retinal Injuries,” an overview paper from April 2015 in Retina Today. The Conclusion section includes this paragraph:- “No definitive experimental study, case report, or animal model has shown improvement in these injuries with any type of treatment, but typically these patients are treated with a short course of corticosteroids or nonsteroidal antiinflammatory drugs. Secondary choroidal neovascularization has been treated successfully with intravitreal anti-VEGF agents.”
Another resource is “Shedding Some Light on Laser Pointer Eye Injuries”, a paper from Pediatric Emergency Care, September 2007, Vol. 23, Issue 9, pp 669-672. The entire article is available online here for $35 (registration also required which takes a few minutes). The following is from the abstract:- ”Results: The scientific literature finds that laser eye injuries are uncommon from use of nonindustrial lasers. Furthermore, an eye injury from a regulated Class 2 or Class 3A by a transient sweep across the line of vision does not result in injury, but injury can occur with a direct intentional prolonged exposure. Conclusions: Patient's history of the length and type of laser exposure is important. A significant direct eye exposure to a laser, persistent after images, and decreased visual acuity should initiate urgent referral to an ophthalmologist for further ophthalmologic testing. Brief laser exposure or indirect exposures with complaints of headaches or blurry vision require other diagnostic explanations.”
